Retina Dekolmanı
Retina Dekolmanı
Hakkında Bilmeniz Gerekenler
Özel Karşıyaka Göz Hastanesi Göz Hastalıkları Uzmanı Doç. Dr. Göktuğ Seymenoğlu retina dekolmanlarının körlüğe kadar ilerleyebileceğini söyledi. Retinanın göz küresinin iç yüzeyini bir kağıt gibi kapladığını belirten Doç. Dr. Göktuğ Seymenoğlu, görme hücrelerinden oluşan bir ağ tabakası olan retinada oluşan hastalıkların, görme düzeyini doğrudan etkilediğini söyledi. Retinada birçok hastalığın oluşabileceğine dikkat çeken Doç. Dr. Göktuğ Seymenoğlu, “Ani görme kaybı, kırık, eğri ya da çarpık görme, ışık, şimşek çakmaları, göz önünde oluşan uçuşmalar, göze perde inmesi, gelip geçici ve kısa süreli görme kaybı, görme alanında karanlık bölgeler oluşması gibi belirtiler Retinada bir problem olduğunu gösterebilmektedir. Retina dekolmanı göz küresinin iç yüzünü kaplayan retina tabakasının (ağ tabakası) gözün dış katmanlarından ayrılması sonucu gelişir. Bu ayrılmaya retinada oluşan yırtıklar neden olur. Retina yırtıkları daha çok yüksek miyop hastalarda, delici-kesici göz yaralanmalarından sonra ve katarakt ameliyatından sonra görülebilir. Orta yaş ve üzerinde daha çok olmakla birlikte her yaşta ortaya çıkabilir.
Özel Karşıyaka Göz Hastanesi Göz Hastalıkları Uzmanı Doç. Dr. Göktuğ Seymenoğlu retina dekolmanlarının körlüğe kadar ilerleyebileceğini söyledi. Retinanın göz küresinin iç yüzeyini bir kağıt gibi kapladığını belirten Doç. Dr. Göktuğ Seymenoğlu, görme hücrelerinden oluşan bir ağ tabakası olan retinada oluşan hastalıkların, görme düzeyini doğrudan etkilediğini söyledi. Retinada birçok hastalığın oluşabileceğine dikkat çeken Doç. Dr. Göktuğ Seymenoğlu, “Ani görme kaybı, kırık, eğri ya da çarpık görme, ışık, şimşek çakmaları, göz önünde oluşan uçuşmalar, göze perde inmesi, gelip geçici ve kısa süreli görme kaybı, görme alanında karanlık bölgeler oluşması gibi belirtiler Retinada bir problem olduğunu gösterebilmektedir. Retina dekolmanı göz küresinin iç yüzünü kaplayan retina tabakasının (ağ tabakası) gözün dış katmanlarından ayrılması sonucu gelişir. Bu ayrılmaya retinada oluşan yırtıklar neden olur. Retina yırtıkları daha çok yüksek miyop hastalarda, delici-kesici göz yaralanmalarından sonra ve katarakt ameliyatından sonra görülebilir. Orta yaş ve üzerinde daha çok olmakla birlikte her yaşta ortaya çıkabilir.
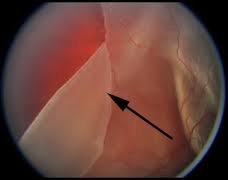
Körlüğe Kadar İlerleyebilir
Retina dekolmanının zamanında ve doğru müdahale edilmediği taktirde körlüğe kadar ilerleyebilecek bir hastalık olduğuna dikkat çeken Doç. Dr. Göktuğ Seymenoğlu, “Retinanın yapışık olduğu tabakadan ayrılması, bu tabaka üzerinde bulunan görme hücrelerinin beslenmesini bozacaktır ve bu hücrelerin ölmesi ile sonuçlanacaktır. Retina dekolmanının makulaya (sarı nokta) ilerlemesi, merkezi görmenin kaybolmasına neden olur. Eğer zamanında müdahale edilmezse Retina başarılı bir şekilde yerine oturtulsa bile, yaşanan zaman kaybı nedeniyle retina üzerindeki görme hücreleri ölür ve geri dönüşümsüz görme kaybı meydana gelir” dedi..
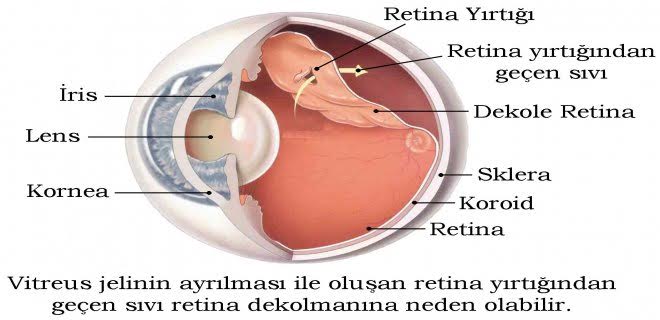
Dışardan Çökertme Yöntemi ile Tedavi
Retina dekolmanı gelişmeden önce sadece retina yırtığı varsa bu genellikle lazer ile bazen de krioterapi (dondurma tedavisi) ile tedavi edildiğini söyleyen Doç. Dr. Göktuğ Seymenoğlu, “Amaç yırtığın dekolmana neden olmadan önce yapıştırılmasıdır. Retina dekolmanı geliştiyse, cerrahi müdahele yani ameliyat gereklidir. Dışardan Çökertme (Skleral Çökertme) Yöntemi, dekole retinayı yapıştırmak için gözün etrafına Retina yırtığı bölgesine denk gelecek şekilde silikondan yapılmış bir bant sarılır. Daha sonra retinadaki yırtık lazer veya krioterapi ile yapıştırılarak kapatılır. Retina altında biriken sıvı da skleradan yapılan küçük bir kesi ile boşaltılabilir. Bant göz etrafında bırakılmasına karşın ağrıya neden olmaz ve dışardan görülmez.